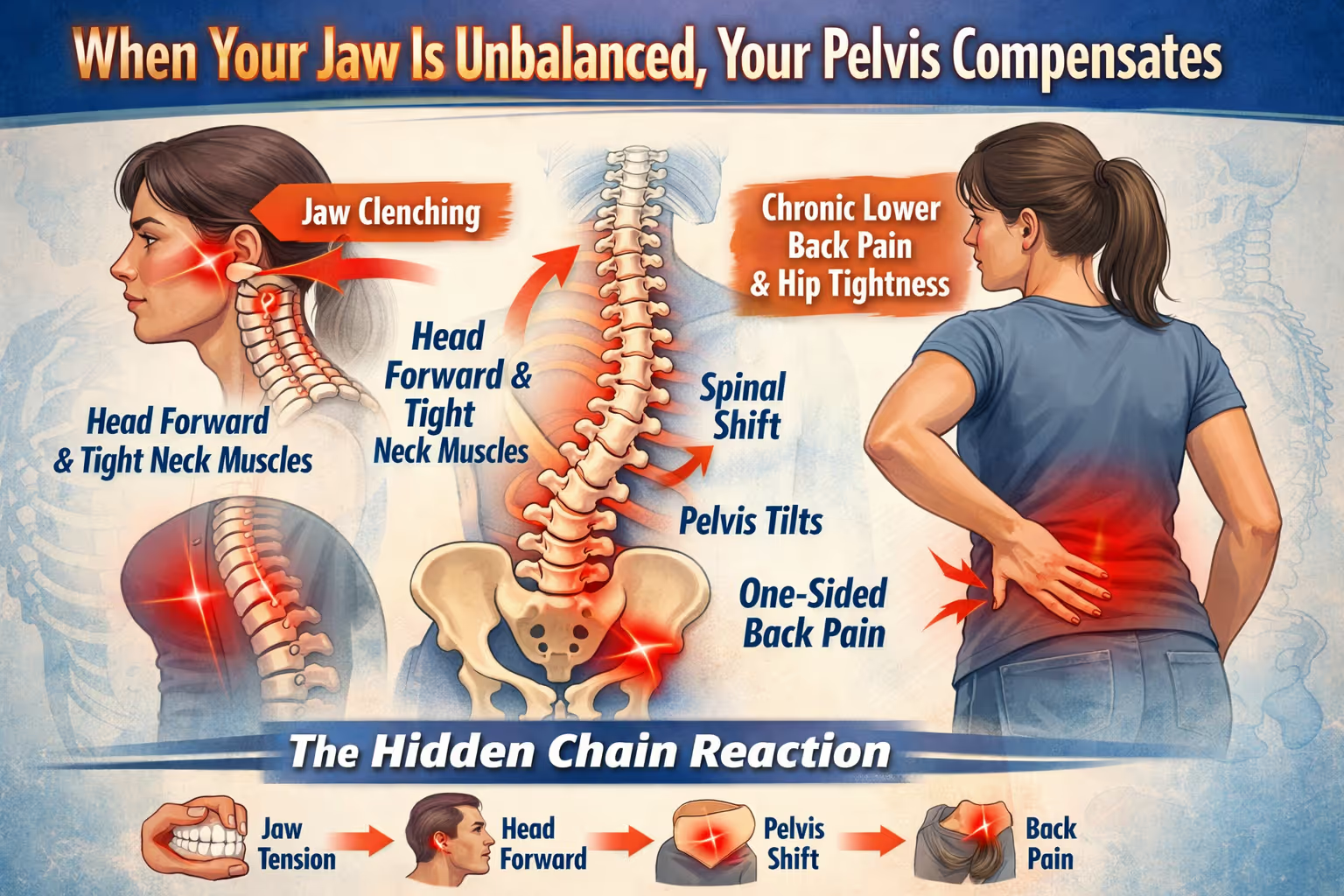
The Hidden Connection Between Jaw Tension, Pelvic Tilt & One-Sided Back Pain
The Pain Isn’t Where You Think It Is
You stretch your hips.
You strengthen your core.
You foam roll your glutes.
You get your pelvis adjusted.
Yet the one-sided lower back pain keeps coming back.
If you’re on Sydney’s Northern Beaches — especially here around Brookvale and Allambie Heights — we see this pattern all the time at Neurohealth Wellness.
The missing piece?
Your jaw.
What if the real driver of your chronic pelvic tilt, SI joint irritation or recurring lower back tightness isn’t your hips at all… but tension you’re holding in your jaw?
Let’s unpack the cascade.
The Cascade: How Jaw Tension Travels Down the Body
When your jaw is unbalanced or chronically clenched, your body compensates in a predictable sequence:
- Jaw imbalance pulls your head forward
- Deep neck muscles tighten to stabilise
- Your spine shifts to keep you upright
- Your pelvis tilts to maintain balance
- One-sided back pain, hip tightness or SI joint dysfunction appears
This is not theory. It’s neurology and biomechanics working together.
Your brain’s priority is balance and survival — not perfect posture.
When one part of the system shifts, the rest of the body adapts.
Why This Happens: The Jaw–Neck–Spine Connection
Your jaw isn’t isolated. It’s deeply integrated with your nervous system and spinal stabilisers.
The temporomandibular joint (TMJ) connects through fascial, muscular and neurological pathways to the upper cervical spine.
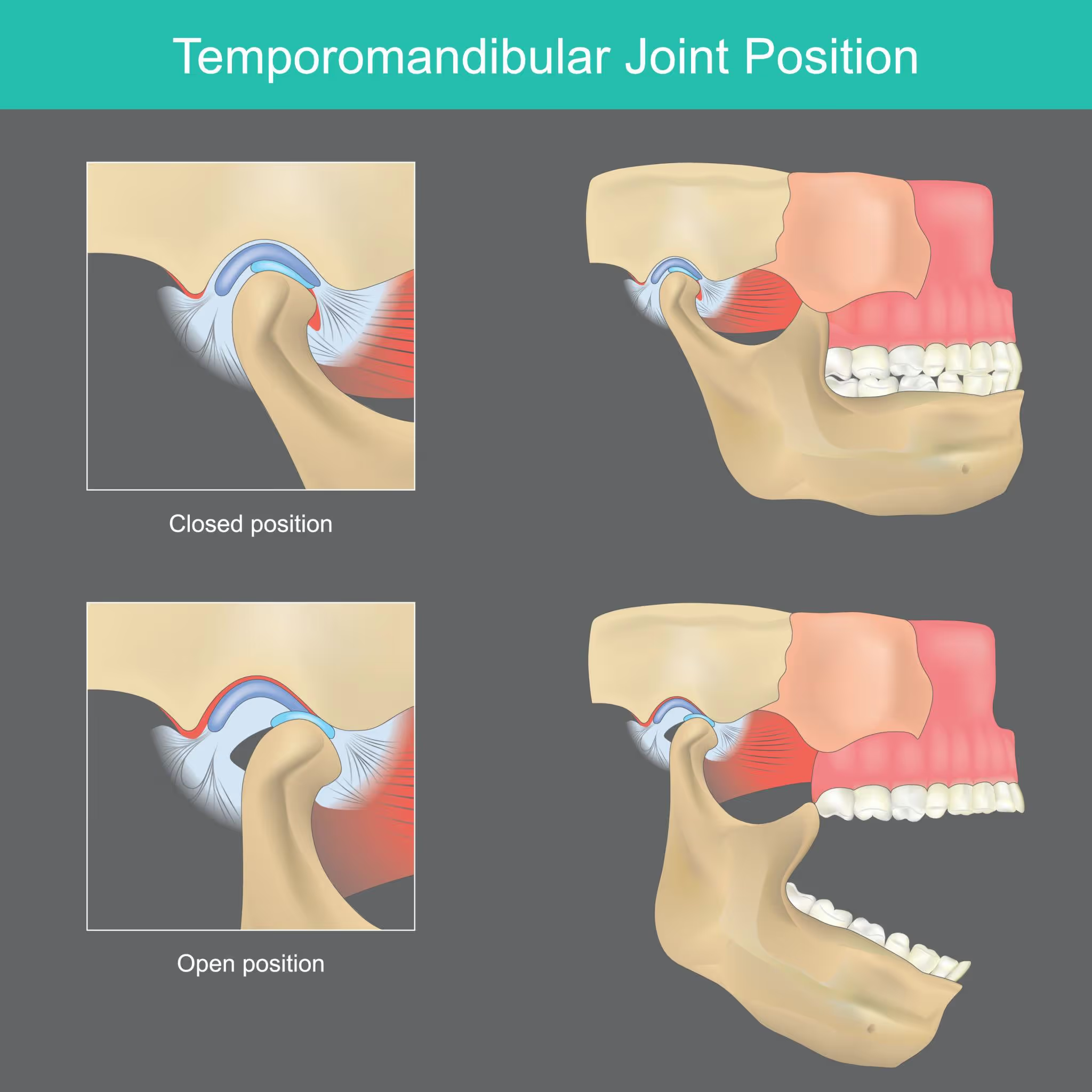
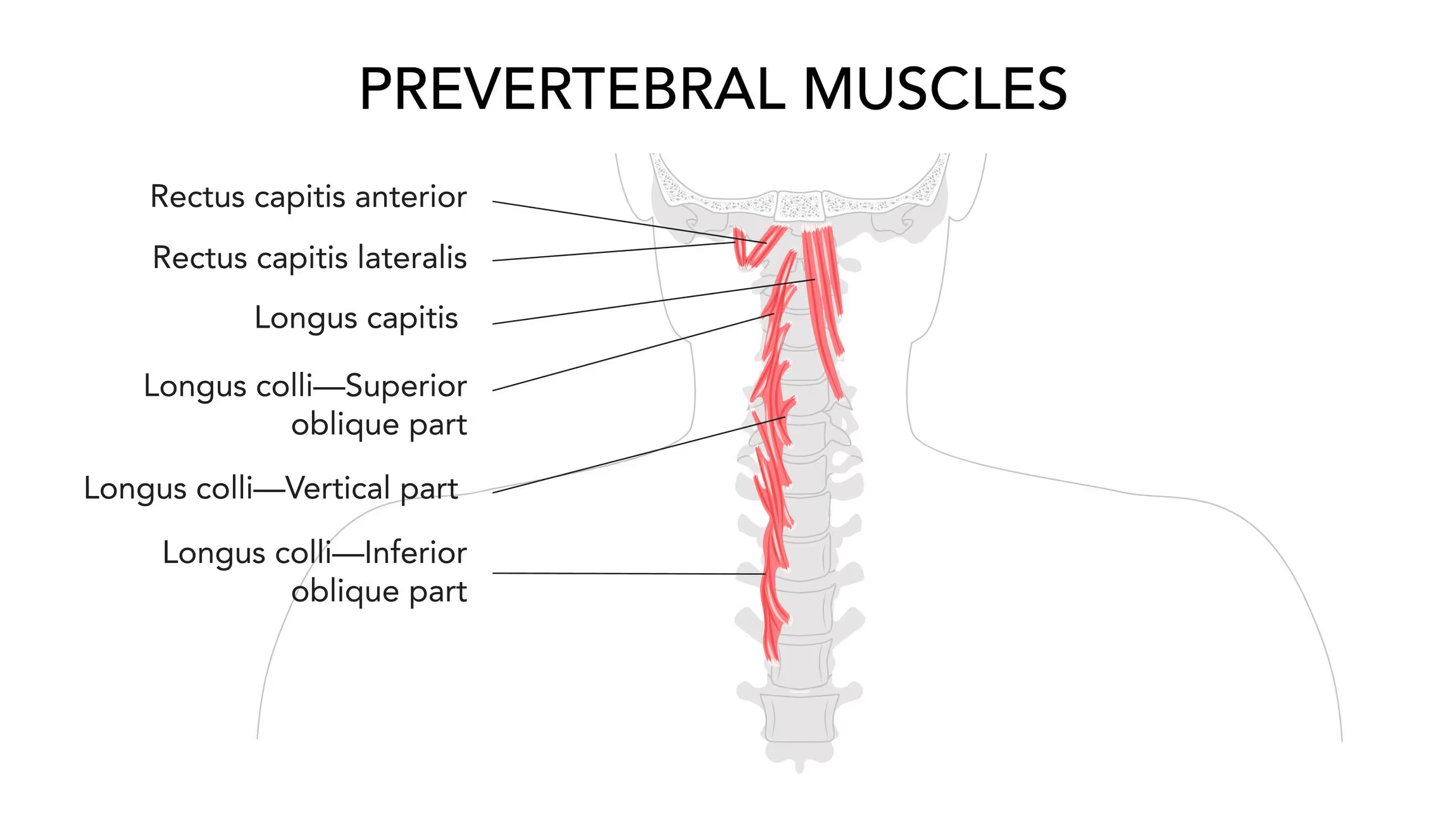

The jaw connects to:
- The suprahyoid and infrahyoid muscles
- Deep neck flexors
- Suboccipital muscles
- Upper cervical spine stabilisers
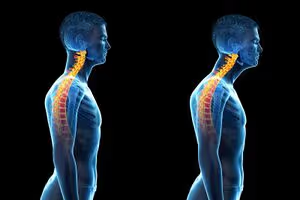
When jaw muscles stay tight — especially from stress-related clenching — they pull the head slightly forward.
That subtle forward shift changes everything.
Your neck muscles tighten to hold your head up.
Your thoracic spine adapts.
Your lumbar spine shifts.
Your pelvis tilts backward to counterbalance.
The brain is constantly recalculating centre of gravity.
And eventually, something starts to hurt.
The Pattern We See Every Week in Clinic
The sequence often looks like this:
Stressed → Clench jaw → Head forward → Pelvis compensates → Chronic pain
Most people treat the end of the chain.
They stretch their hips.
They do glute activation work.
They strengthen their core.
They get pelvic adjustments.
And those things can absolutely help — temporarily.
But if the jaw tension hasn’t changed, the compensation pattern resets.
That’s why the pain keeps returning.
The Chiropractic Bridge: Why This Matters to Your Whole Body
At Neurohealth Wellness, we don’t just look at where it hurts.
We assess how your nervous system is organising your posture.
Because posture isn’t a muscle problem.
It’s a neurological strategy.
When the jaw is chronically clenched — often subconsciously, especially at night — the trigeminal nerve and upper cervical nerves become hyperactive.
That increased neural input alters:
- Head position
- Cervical muscle tone
- Spinal alignment
- Pelvic orientation
Your brain is trying to keep your eyes level and your body upright.
If your head shifts forward from jaw tension, your pelvis will shift backward to maintain equilibrium.
And that’s when:
- One-sided lower back pain develops
- SI joint irritation appears
- Hip tightness doesn’t resolve
- Core strengthening feels ineffective
You can’t out-exercise a neurological compensation pattern.
If you’re dealing with recurring one-sided back pain or pelvic tightness that never fully settles, it may be time to assess the whole chain.
👉 Book a $67 New Patient Chiropractic Assessment with Florian (normally $150) and we’ll evaluate your jaw, posture, spine and pelvic mechanics as one integrated system.
Book online: https://www.neurohealthwellness.com.au/booking
📞 Or call us on (02) 9905 9099
Why Conscious Relaxation Isn’t Enough
Many jaw clenchers know they clench.
They try to relax.
They remind themselves during the day.
They become more aware.
But the real issue?
Most clenching happens subconsciously — especially during stress or sleep.
You cannot consciously override a reflex pattern that’s been wired into your nervous system for years.
To truly break the cycle, the jaw must stop clenching automatically — even when you’re not thinking about it.
When jaw tension releases at a reflex level:
- The head repositions naturally
- The upper cervical spine decompresses
- Muscle tone normalises
- The pelvis stops compensating
And often, the one-sided back pain fades — not because the back was treated directly, but because the upstream trigger stopped firing.
The Stress Factor: Why It’s So Common
Living and working in fast-paced environments — whether commuting through Sydney, running businesses, managing families or training hard at the gym — increases sympathetic nervous system activity.
Stress drives jaw clenching.
Jaw clenching drives head-forward posture.
Head-forward posture drives pelvic compensation.
This is why high-performing professionals, athletes and even teenagers studying for exams can develop unexplained back or hip pain.
The jaw is often the silent contributor.
Prevention Over Reaction: The Neurohealth Ethos
At Neurohealth Wellness on Sydney’s Northern Beaches, our focus is not just symptom relief.
It’s breaking patterns before they become chronic.
That means:
- Assessing jaw tension and TMJ mechanics
- Evaluating cervical spine function
- Looking at pelvic balance
- Analysing posture under load
- Addressing nervous system tone
We don’t chase pain.
We find the driver.
And often, that driver isn’t where you feel it.
What About Jaw Retraining?
There are emerging approaches that aim to retrain jaw position reflexively rather than relying on conscious relaxation.
At Neurohealth, we assess whether jaw tension is part of your pattern and guide you through appropriate strategies, whether that includes manual care, postural retraining, breathing work or collaborative referral if needed.
Every patient is individual. The pattern must be assessed, not assumed.
If you have:
- One-sided lower back pain
- Chronic SI joint irritation
- Persistent hip tightness
- Posture that keeps collapsing forward
- A history of jaw clenching or grinding
It may be time to stop treating the pelvis in isolation.
👉 Book your $67 New Patient Chiropractic Assessment today with Florian
🌐 www.neurohealthwellness.com.au/booking
📞 (02) 9905 9099
📍 33–35 Kentwell Rd, Allambie Heights (Northern Beaches, Sydney)
Let’s assess the whole chain — from jaw to pelvis — and rebalance your body properly.
References
- Armijo-Olivo, S., Silvestre, R. A., Fuentes, J. P., et al. (2011).
Association between temporomandibular disorders and cervical spine disorders: A systematic review.
Journal of Oral Rehabilitation, 38(6), 442–469. https://doi.org/10.1111/j.1365-2842.2010.02182.x - Cuccia, A. M., & Caradonna, C. (2009).
The relationship between the stomatognathic system and body posture.
Clinics, 64(1), 61–66. https://doi.org/10.1590/S1807-59322009000100011 - Budelmann, K., von Piekartz, H., & Hall, T. (2013).
Is there a relationship between craniocervical posture and temporomandibular disorders? A systematic review.
Manual Therapy, 18(3), 209–218. https://doi.org/10.1016/j.math.2012.11.004 - Michelotti, A., Farella, M., Martina, R., et al. (1999).
Effects of occlusal interference on habitual activity of jaw and neck muscles.
Journal of Oral Rehabilitation, 26(8), 644–649. https://doi.org/10.1046/j.1365-2842.1999.00443.x - Fernández-de-las-Peñas, C., Alonso-Blanco, C., Cuadrado, M. L., et al. (2006).
Forward head posture and neck mobility in chronic tension-type headache: A blinded controlled study.
Cephalalgia, 26(3), 314–319. https://doi.org/10.1111/j.1468-2982.2005.01024.x - Olivo, S. A., Bravo, J., Magee, D. J., et al. (2010).
The association between head and cervical posture and temporomandibular disorders: A systematic review.
Journal of Orofacial Pain, 24(1), 9–23. - Kang, J. H., Park, R. Y., Lee, S. J., et al. (2012).
The effect of forward head posture on postural balance in long-time computer-based workers.
Annals of Rehabilitation Medicine, 36(1), 98–104. https://doi.org/10.5535/arm.2012.36.1.98 - Saito, E. T., Akashi, P. M. H., & Sacco, I. C. N. (2009).
Global body posture evaluation in patients with temporomandibular joint disorder.
Clinics, 64(1), 35–39. https://doi.org/10.1590/S1807-59322009000100007