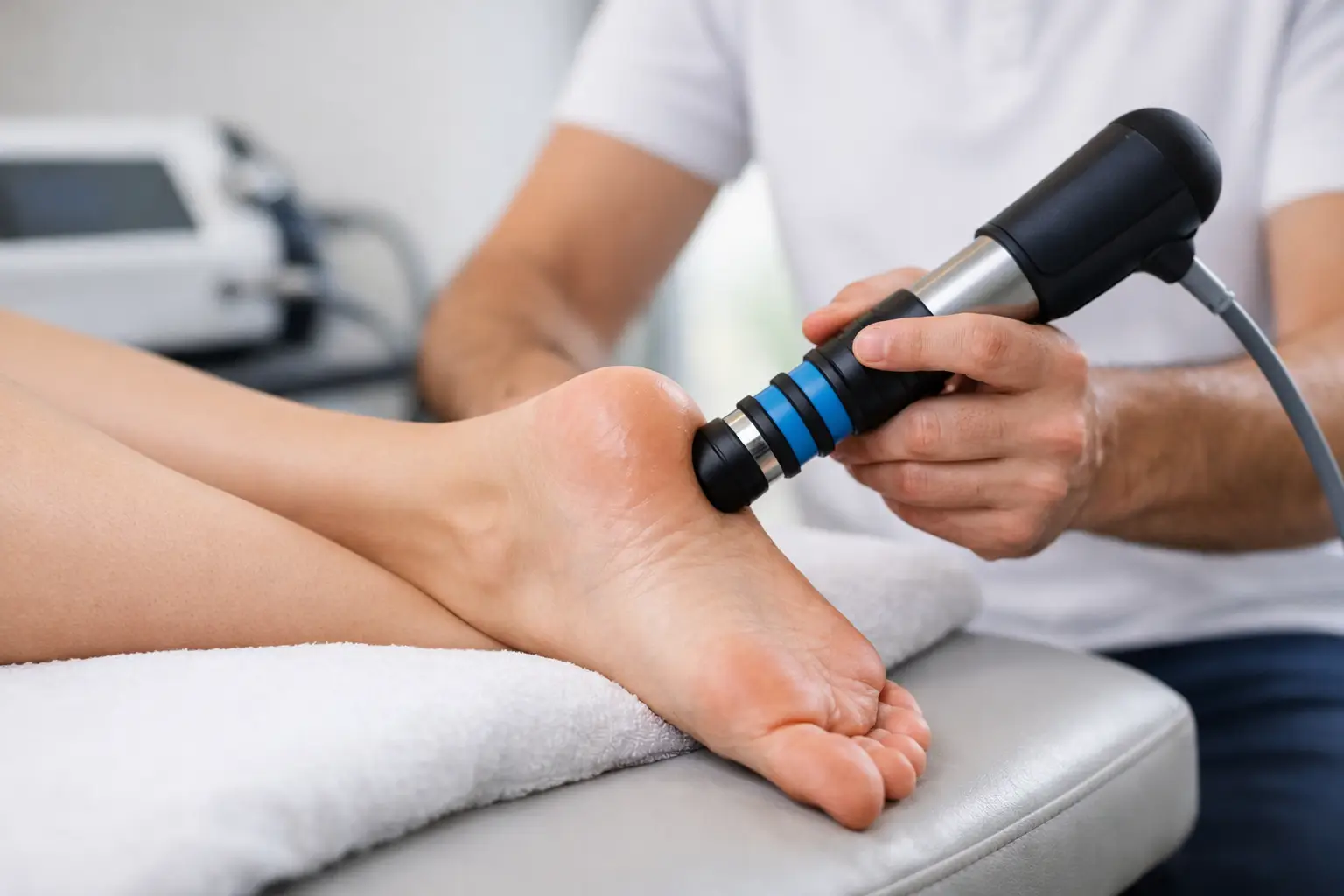
That sharp heel pain when you first step out of bed can change the whole rhythm of your day. If every morning starts with a wince, or a walk along the Northern Beaches feels harder than it should, shockwave therapy for plantar fasciitis may be one of the treatment options worth considering.
Plantar fasciitis is one of the most common causes of heel pain, especially in active adults, runners, people who spend long hours on their feet, and office workers who move poorly after sitting for much of the day. The plantar fascia is a strong band of tissue that runs along the bottom of the foot, connecting the heel to the toes. When that tissue becomes irritated or overloaded, even simple movement can feel frustrating.
At our clinic, we take a broader view of this kind of pain. The foot matters, of course, but so do the calf, ankle, hips, posture, training load, footwear, recovery habits and the way your whole body is moving. That is often where better long-term results come from.
What is shockwave therapy for plantar fasciitis?
Shockwave therapy is a non-invasive treatment that uses acoustic waves to stimulate the affected tissue. In plain terms, it delivers targeted pulses into the sore area to encourage circulation, support tissue repair and help reduce pain.
For plantar fasciitis, the treatment is usually applied around the heel and along the plantar fascia where tenderness is most obvious. Sessions are relatively quick, and many people are able to return to normal daily activity straight after treatment. It is not surgery, and there is no need for anaesthetic or lengthy downtime.
People are often drawn to shockwave because it can help when heel pain has lingered for weeks or months and basic self-care has not been enough. That said, it is not a magic fix. The best outcomes usually happen when it is part of a personalised treatment plan rather than a stand-alone approach.
Why plantar fasciitis keeps coming back
Heel pain rarely appears out of nowhere. Sometimes it starts after a jump in running distance, a new sport, long days standing at work or unsupportive footwear. Other times it builds gradually, especially when the body has been compensating for restricted ankle movement, tight calves, poor load management or weakness through the feet and legs.
This is why some people get temporary relief but not lasting change. If the inflammation settles for a short time but the underlying strain is still there, symptoms can return as soon as life gets busy again.
From a holistic care perspective, it helps to ask better questions. Is the foot absorbing more load than it should? Is there stiffness higher up the chain? Has stress, poor sleep or under-recovery affected healing? Is your training or work routine simply asking too much of irritated tissue? These details matter.
How shockwave therapy may help
Shockwave therapy for plantar fasciitis is often used to support the body's natural repair process. The acoustic waves are thought to help stimulate blood flow and cellular activity in tissue that may not be healing efficiently. It can also help desensitise painful areas, which may make walking and exercise more comfortable.
For many people, the appeal is that treatment can be targeted and practical. You do not need to stop life completely, and there is usually minimal interruption to work, family responsibilities or training. For active people, that can make a big difference.
Still, there are trade-offs. The treatment can feel uncomfortable while it is being done, especially over a very tender heel. Some people improve quickly, while others need a series of sessions before change is noticeable. Chronic cases often take longer than recent flare-ups.
Who may be a good fit for treatment?
Shockwave therapy may suit people who have plantar fasciitis that has not settled with rest, stretching, massage, shoe changes or simple home care. It can also be useful for people who want a non-surgical option and are looking for a treatment that supports tissue healing while allowing them to stay as active as possible.
It may be especially relevant for runners, gym-goers, walkers, tradies, nurses, hospitality workers and parents who spend long hours on their feet. We also often see heel pain in people who are less active but dealing with tight calves, reduced mobility or long periods of sitting followed by sudden bursts of movement.
A proper assessment is still important. Not every case of heel pain is plantar fasciitis. Sometimes the pain is linked to a nerve issue, fat pad irritation, Achilles involvement or a different foot condition. Getting the diagnosis right is the first step.
What to expect from shockwave therapy sessions
Your practitioner will begin with a detailed assessment, not just of the painful spot but of how your body is functioning as a whole. That may include looking at ankle mobility, calf tension, gait, footwear, training habits and any contributing issues through the knees, hips or lower back.
During treatment, gel is applied to the area and a handheld device delivers pulses to the affected tissue. Most sessions are short. The sensation is usually described as intense but manageable, and the exact settings can be adjusted depending on your sensitivity and the condition of the tissue.
Afterwards, it is common to feel mild soreness for a day or two. That does not necessarily mean anything is wrong. It is simply part of how the area responds. Your practitioner may advise temporary adjustments to running, walking volume or high-impact exercise while the tissue settles.
Why a combined approach often works better
This is where many people get the best value from care. Shockwave can be very helpful, but if the foot keeps being overloaded, results may be limited.
A more complete plan may include hands-on treatment to release tight calves and foot muscles, myotherapy or remedial massage to improve tissue quality, acupuncture for pain relief, and exercise-based rehabilitation to improve strength and load tolerance. In some cases, chiropractic care may also help if lower limb mechanics or spinal and pelvic function are contributing to compensation patterns.
Supportive advice around footwear, stretching, pacing and return to exercise also matters. If you are an athlete, your plan should account for performance goals, not just pain levels. If you are a busy parent or office worker, it needs to fit real life. Good care should feel tailored, not generic.
How long does it take to feel better?
It depends on how long the problem has been there, how irritated the tissue is and whether the causes are being addressed at the same time. Some people notice a shift after a couple of sessions. Others improve more gradually over several weeks.
Long-standing plantar fasciitis usually needs patience. If you have been limping for months, changing that pattern takes time. The goal is not only to calm the pain but to help your foot handle load better so symptoms are less likely to keep returning.
This is also why expectations matter. Treatment should move you in the right direction, but healing is rarely perfectly linear. You may have better days and flatter days along the way.
When to seek help sooner
If heel pain is affecting your walking, stopping you from exercising or lingering despite rest, it is worth having it assessed. The earlier you understand what is driving the pain, the easier it is to build the right treatment plan.
You should also seek guidance if the pain is worsening, spreading, or paired with numbness, significant swelling or a sudden change after injury. Not every sore foot needs shockwave, and not every heel pain story follows the same pattern.
At Neurohealth Wellness, care is built around the person, not just the label. That means looking at how your body moves, what your week really looks like, and what kind of support will help you heal well and stay well.
If plantar fasciitis has been wearing you down, there is value in getting clear, practical advice and a plan that supports both relief and recovery. The right treatment should help you move with more confidence, not just get through the day.